Research with a practical lens
Whipple named a BIRCWH scholar for research with older adults with type II diabetes
November 14, 2023
Susan Maas

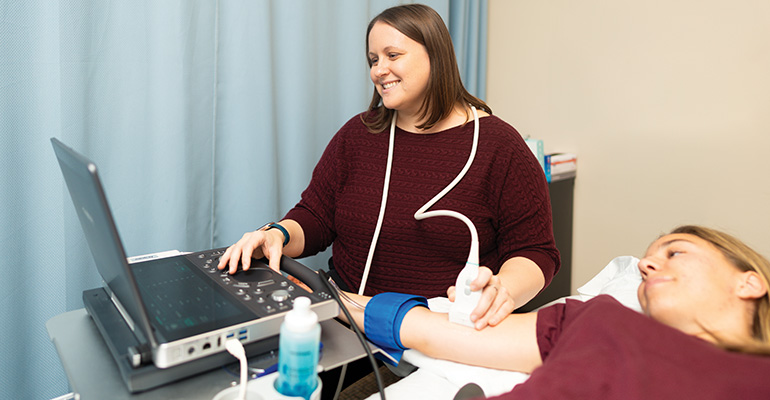
Assistant Professor Mary Whipple’s research focuses on strategies that are simple yet impactful to help older adults move more.
A cascade of health crises that rapidly shrunk her once-independent grandmother’s life—beginning with poorly managed type II diabetes—helped lead Assistant Professor Mary Whipple, PhD, RN, PHN, FSVM, to nursing.
It’s also directly related to Whipple’s latest research, for which she was named a Building Interdisciplinary Research Careers in Women’s Health (BIRCWH) scholar by the National Institutes of Health this year. Whipple is studying whether and how breaking up sedentary behavior in older people with type II diabetes might improve vascular function. The BIRCWH program offers mentorship, networking, professional development, and assistance with manuscript and grant writing.
“We already know that sitting too much is bad,” says Whipple. Yet evidence suggests that interspersing intense workouts with long periods of sitting isn’t the answer to better health outcomes, Whipple explains. Her research seeks to establish whether breaking up sedentary periods with shorter, more frequent bits of exercise might have a meaningful impact beyond simply exercising a certain number of hours each week.
Breaking up ‘sedentary behavior’
While some other studies look at high-intensity interval training, Whipple says, “I’m interested in things that are practical and can fit into daily life. We hear a lot from people about how challenging exercise can be. Some people say that it feels a little bit overwhelming, like, ‘I don’t have an hour, or half an hour.’”
But what about a very short walk, or a few squats, or five minutes of cycling? Whipple’s project will explore whether exercise spread out in small intervals throughout the day can yield better vascular outcomes than one longer exercise session. Participants will wear monitors that measure sedentary behavior and physical activity. Each participant will try three different types of activity: exercising for short intervals multiple times daily, exercising for a longer period once daily, and remaining sedentary.
Whipple and her team will measure participants’ blood pressure, and they’ll use an ultrasound technique called flow-mediated dilation (FMD) to also measure changes in the diameter of patients’ arteries in the three different conditions. She’s enrolling women and men, age 60 and older, with type II diabetes in the study. “There’s reason to believe there might be some differences in women and men because of menopause and the way it impacts cardiovascular health,” she says. The three-year grant began this summer. Whipple anticipates preliminary findings in two years.
Whipple — who joined the nursing faculty in 2022 — returned to Minnesota after a postdoctoral fellowship in geriatrics at the University of Colorado School of Medicine. One of her projects there involves examining seniors’ sense of meaning and mood in relationship to physical activity: “We’re having folks wear activity monitors and then sending them quick surveys asking, ‘In this moment, how do you feel, in terms of tired, anxious, upset, or happy?’”
Keeping seniors healthier, longer
Having grown up in Rochester, Minnesota, home of the Mayo Clinic, probably had something to do with Whipple’s attraction to health care (in fact, Whipple began college in Iowa as a premed student, and worked as a research coordinator at Mayo after graduation). However it was her mother’s bout with breast cancer years ago, and especially her grandmother’s steep decline after being injured in a fall, that more directly led to Whipple’s focus on seniors, diabetes, cardiovascular health and physical fitness.
“She fell in her home and had a fracture,” Whipple says. “Then she had multiple infections, and never really walked again. She had been such an independent woman. The idea of a fall and how it can so dramatically diminish that independence is something that’s driven me to focus on older adults and strategies that maybe are really simple, but could be impactful.”
Whipple is glad to be doing more teaching; her two-and-a-half years in Colorado didn’t include much teaching. She teaches research as well as honors thesis, and this past spring taught a grant writing course in the PhD program. Whipple also serves as an associate editor for Vascular Medicine. “It’s been fun being the only nurse on that team,” she says. “I’ve learned a lot from that process. It’s helped me become a better writer by learning to be a better reviewer. That’s something that I share with students: there’s a lot of value in being a reviewer.”
It’s an honor to be back at the U of M, Whipple says. “I’m proud to be here on the faculty—being in the place where I got my BSN, where I got my PhD, is really cool. To be able to be part of giving the kind of mentorship that I got when I was a student, and that I still get, is wonderful. It’s a great place to be.”
Watch Mary Whipple talk about the ways a PhD in Nursing can be utilized to improve health at z.umn.edu/Whipple


